Cancer Diagnostics in Healthcare: Detecting the Undetectable
May 13, 2026
Table of Contents
Cancer has long been called a silent killer, not because it lacks signs, but because those signs often arrive too late. For decades, oncology was dominated by a reactive model: patients presented with symptoms, received a diagnosis, and began treatment at an advanced stage when outcomes were already compromised. Today, that narrative is being rewritten. Early-stage cancer diagnosis can increase five-year survival rates dramatically. For breast cancer, early detection pushes survival rates above 99%; for lung cancer, catching the disease at Stage I versus Stage IV means the difference between a 60% survival rate and less than 6%. The numbers make one thing undeniable: when we detect cancer earlier, we save more lives.
What’s driving this shift isn’t just clinical vigilance. It’s a convergence of molecular biology, artificial intelligence, and precision medicine that is fundamentally transforming the diagnostic landscape. Cancer diagnostics in 2026 is no longer just about imaging a tumor; it’s about reading the body’s earliest distress signals, often before a single cell has formed a detectable mass. The traditional toolkit of cancer diagnostics has historically included:
Downloads
Click Here To Get the Article in PDF
Recent Articles
- Monteris Smallest Brain Laser Probe Launch; Vesica Health’s AssureMDx Test Launch; Anaut’s Eureka...
- Generative AI in Drug Discovery: Applications and Market Impact
- GE HealthCare, DePuy Synthes Announced Collaboration; Eko Health Launched CORE 500 Digital Stetho...
- AI Hospitals of the Future–Where Robotics, Predictive Analytics, and Compassion Converge
- iRhythm’s Zio® AT Device Improvements Receive FDA Clearance; Epitel Adds REMI AI Device to Portfo...
- Imaging techniques such as X-rays, CT scans, MRI, and PET scans to visualize tumors
- Tissue biopsies to analyze cellular morphology and confirm malignancy
- Endoscopic procedures for GI, lung, and bladder cancers
- Blood-based tumor markers like PSA (prostate-specific antigen) and CA-125 (ovarian cancer)
- Genetic testing for hereditary cancer predispositions, such as BRCA1/2 mutations
Each method has served an important role, but each also carries limitations, from invasiveness and radiation exposure to low sensitivity in early-stage disease. The next generation of diagnostics is focused on overcoming exactly these barriers.
The Rise of Liquid Biopsies
Perhaps no innovation has generated more excitement in oncology diagnostics than the liquid biopsy. The concept is elegant: instead of surgically extracting tumor tissue, clinicians analyze a simple blood sample for circulating tumor DNA (ctDNA), circulating tumor cells (CTCs), or tumor-derived exosomes.
Liquid biopsies work because tumors shed genetic material into the bloodstream. By isolating and sequencing this cell-free DNA, oncologists can identify cancer-specific mutations, monitor treatment response in real time, and detect residual disease after therapy, all without ever touching the tumor itself.
The clinical implications are profound. Liquid biopsies are increasingly being used to:
- Detect early-stage cancers before symptoms appear, even across multiple cancer types simultaneously (multi-cancer early detection, or MCED)
- Identify actionable mutations for targeted therapy selection
- Monitor for acquired resistance mutations during treatment
- Detect minimal residual disease (MRD) post-surgery to predict recurrence risk
Companies like Grail, Myriad Genetics Inc, Exact Sciences Corporation, Biocartis, Sysmex Corporation, Thermo Fisher Scientific Inc, Biocept Inc, Agilent Technologies Inc, MDx Health, Neogenomics Laboratories, F. Hoffman La Roche Ltd, Guardant Health, Bio-Techne, Illumina Inc, QIAGEN, Lucence Health Inc, Personal Gemone Diagnostics Inc, SAGA Diagnostics, Agena Bioscience Inc, The Menarini Group, MiRXES Pte Ltd., and others have spearheaded the commercialization of these platforms, and regulatory approvals have begun to follow. The Galleri test by Grail, designed to detect over 50 cancer types from a single blood draw, represents a new paradigm: population-level cancer screening that was previously unimaginable.
Challenges remain around sensitivity, specificity, and reimbursement, particularly for early-stage detection, where ctDNA levels are extremely low. But the trajectory is clear: liquid biopsies are moving from specialty oncology clinics to mainstream diagnostic workflows.

AI and Advanced Imaging in Cancer Diagnostics
Radiology has always been foundational to cancer diagnosis, but human interpretation of complex imaging is inherently limited by volume, fatigue, and inter-reader variability. Artificial intelligence is changing that equation.
AI-powered imaging platforms use deep learning algorithms trained on millions of annotated scans to identify subtle radiological features that human eyes might miss. In mammography, AI tools have demonstrated sensitivity and specificity comparable to, and in some studies exceeding, experienced radiologists. In lung cancer screening via low-dose CT, AI algorithms can flag early nodules with remarkable precision, helping to reduce the false-positive burden that has historically made lung screening programs difficult to scale.
Beyond detection, AI is adding a new dimension called radiomics, the extraction of quantitative features from imaging data that correlate with tumor biology, genetic mutations, and prognosis. A radiomics signature derived from a CT scan can, in some cases, predict whether a tumor harbors specific driver mutations without requiring a biopsy. This non-invasive molecular profiling represents a significant leap in diagnostic efficiency.
AI is also accelerating pathology. Digital pathology platforms now allow whole-slide imaging to be analyzed algorithmically, identifying histological patterns, grading tumors, and even predicting immunotherapy response from routine H&E stains, tasks that previously required specialized molecular assays. The integration of AI into the diagnostic ecosystem is not replacing pathologists and radiologists; it is amplifying their capabilities and enabling them to work at scale.
Biomarkers and Precision Medicine in Cancer Diagnostics
Cancer is not one disease; it is thousands of molecularly distinct diseases that happen to share the characteristic of uncontrolled cellular growth. Precision medicine acknowledges this reality by tailoring diagnosis and treatment to the specific molecular profile of an individual’s tumor.
Biomarker testing has become the gateway to precision oncology. Genomic profiling through next-generation sequencing (NGS) can now analyze hundreds of cancer-relevant genes simultaneously, identifying driver mutations, copy number alterations, fusions, and microsatellite instability (MSI) status in a single assay. These findings directly inform treatment decisions: EGFR mutations in lung cancer direct clinicians toward osimertinib, HER2 amplification opens the door to trastuzumab-based regimens, and high tumor mutational burden (TMB) predicts response to immune checkpoint inhibitors.
Beyond genomics, the biomarker landscape now encompasses:
- Proteomics, analyzing protein expression patterns associated with malignancy
- Epigenomics, detecting cancer-specific methylation signatures in circulating DNA
- Transcriptomics, gene expression profiling to classify tumor subtypes and predict prognosis
- Metabolomics, identifying cancer-associated metabolic shifts in blood or urine
Multi-omic integration, combining data from several of these domains, is emerging as the frontier of diagnostic precision. By building a comprehensive molecular portrait of a patient’s cancer, clinicians can move beyond treating the tissue of origin and instead target the specific molecular vulnerabilities driving disease progression.
Challenges That Still Remain in Cancer Diagnostics
For all its promise, cancer diagnostics still faces significant hurdles that prevent the full potential of these technologies from reaching patients equitably and efficiently. Sensitivity and false positives remain a core challenge, particularly in early detection. Multi-cancer early detection tests must balance catching early disease against generating a flood of false alarms that lead to unnecessary procedures, patient anxiety, and healthcare system strain. Refining specificity without sacrificing sensitivity is an ongoing scientific challenge.
Accessibility and cost create sharp disparities. Advanced genomic profiling, liquid biopsy platforms, and AI-enabled diagnostics are primarily available in high-income countries and major academic medical centers. In low- and middle-income countries, where cancer incidence is rising, these tools remain largely out of reach. The MENA region, for instance, has made strides in healthcare infrastructure investment, but diagnostic equity remains a work in progress.
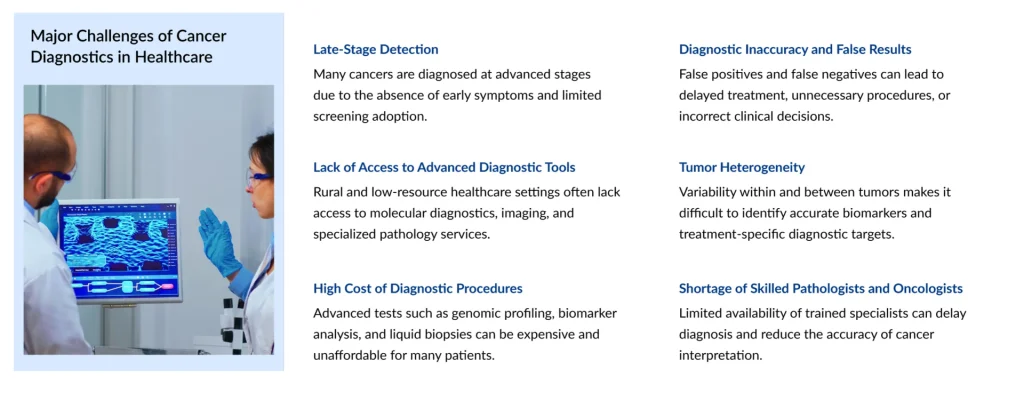

Regulatory and reimbursement frameworks have struggled to keep pace with innovation. Companion diagnostics and novel biomarker assays require rigorous validation and regulatory clearance, a process that can lag years behind the science. Meanwhile, inconsistent payer coverage for NGS testing, liquid biopsies, and MCED screening continues to limit adoption even in markets where these technologies are approved.
Data standardization and interoperability present a systems-level challenge. AI models are only as good as the data they’re trained on, and fragmented healthcare data ecosystems make it difficult to build and validate diagnostic algorithms across diverse populations. Ensuring that AI-based diagnostic tools perform equitably across racial, ethnic, and demographic groups requires diverse, representative training datasets, a standard the field is still working toward.
The Road Ahead
The future of cancer diagnostics is not a single breakthrough; it is the compounding effect of many converging innovations working in concert. Multi-cancer early detection will likely become a standard component of annual preventive health screenings within the next decade, functioning much like today’s cholesterol or blood pressure tests. AI will become embedded in pathology and radiology workflows, not as a novelty, but as a standard of care infrastructure.
Theranostics, the integration of diagnostics and therapeutics, will blur the line between detecting and treating cancer. Radiolabeled molecules that simultaneously identify and destroy cancer cells represent a paradigm where diagnosis and therapy become a single, seamless act. FDA approvals in this space, such as lutetium-177 PSMA for prostate cancer, offer a glimpse of where the field is headed.
Perhaps most significantly, the shift from detection to interception is underway. Cancer interception, identifying and eliminating pre-malignant cells before they become invasive, represents the true culmination of early detection science. Clinical programs targeting precancerous lesions in the lung, colon, esophagus, and pancreas are building the evidence base for a future where cancer is caught not at Stage I, but at Stage 0 or even before.
The challenge facing the healthcare and diagnostics industry is not whether these technologies will work; the science increasingly confirms that they do. The challenge is translating laboratory excellence into a scalable, accessible, and affordable clinical reality. That is a challenge not just for scientists, but for healthcare systems, policymakers, industry leaders, and patient advocates working together to ensure that the undetectable becomes, finally and reliably, detected.

Downloads
Article in PDF
Recent Articles
- AI in Cancer Diagnostics: Paving the Way for Early Detection and Precision Treatment
- Alcon’s Dry Eye Treatment Device; I-VASC Secures Series A Funding; Paige’s AI Medical Device Soft...
- Quest Introduced Consumer-Initiated Blood Test for Alzheimer’s Disease Risk Assessment; DuP...
- Edwards’s Pascal Precision System; Abbott’s New Spinal Cord Stimulation Device; Imagin to A...
- Collagen Matrix FDA 510(k) approval for Fibrillar Collagen Wound Dressing; Roche’s cancer diagnos...